Broken Teeth
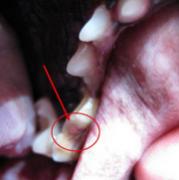
Broken Teeth
Like people, our pets are prone to dental disease. Pet Dental Month, in February, focuses on the importance of controlling and preventing dental disease in our cats and dogs. Untreated dental disease is associated with both infection and pain. Recent studies in people and dogs show that untreated infection in the mouth has also been linked to infections in other parts of their bodies.
Many pets present to the veterinarian with broken teeth. Traditionally, a veterinarian might say, “it’s not bothering the dog or cat so we’ll leave it alone.” If my own dentist told me that regarding one of my own teeth, I’d be looking for a new dentist.
Identifying the Issue
How do we know if a broken tooth is painful? Dogs and cats don’t have the ability to communicate that, but often their teeth hurt in the same way that our teeth can. There are several things we can do to access the viability of a tooth that has been broken. First, if there is obvious pulp exposure, then we know that tooth is dead or is dying, depending upon how long it’s been broken. Pulp is a combination of nerves and blood vessels that live within the center of a tooth. Once the pulp is exposed to the outside world, it rapidly becomes infected and that tooth will die over several weeks to months.
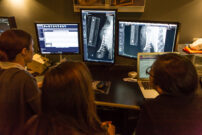
When an animal is under anesthesia, there are radiographic changes that may be seen in a non-vital (dead) tooth. As we age and our teeth mature, the body constantly produces new layers of dentin along the outer walls of the “pulp chamber.” As an animal ages, the pulp chamber diameter becomes smaller and smaller. A tooth with a dilated pulp chamber as seen on x-rays indicates that that particular tooth is non-vital. Also, over time, a dead tooth may develop changes around the root of the tooth seen on x-rays called a periapical lucency (see image on left). This is an area seen around the root tip that usually represents and infection from bacteria that has invaded into the pulp chamber of the tooth, or a cyst developing from inflammation associated with the dead pulp leaking into the bone around the root of the tooth.
Any teeth with pulp exposure, dilated pulp chambers or a periapical lucency should be treated and there is a likelihood that this tooth may be painful to a pet. There are multiple treatment options, although “leaving it alone,” is not in the pet’s best interest.
Saving the Tooth
The option to save the tooth involves endodontic or root canal therapy. First the tooth is evaluated to make sure there is no concurrent disease of the tooth. This includes periodontal disease, fractures below the gum line or advanced destruction of the tooth root. The tooth root must also be mature enough to be treated with endodontic therapy. Endodontic therapy involves cleaning out the pulp chamber of the tooth with a combination of filing and flushing with a disinfectant. Next the tooth is filled with a sealant to prevent the leakage of bacteria through the canal of the tooth. Finally, a filling, or “restoration,” is placed on the opening of the tooth to also prevent bacterial leakage into the pulp chamber. If performed correctly, endodontic therapy is highly effective at salvaging broken teeth with pulp exposure. Endodontic therapy does require follow up care with dental x-rays to make sure the therapy is successful and that the restorations remain intact.
If a fractured tooth is immature, the root is not fully developed, and the fracture is very recent, then a broken tooth may be treated with a procedure called a vital pulpotomy and direct pulp capping. The goal of this procedure is to keep the tooth alive long enough to allow the tooth to mature to a point where endodontic therapy can be performed. If the fracture is not very recent, then a procedure called apexogenesis may be performed to encourage enough maturation of the tooth root to perform endodontic therapy.
Extracting the Tooth
The other treatment option is extraction therapy. This involves removal of the affected tooth. This may be relatively simple or may involve surgery, depending upon which tooth is involved. After the extraction of broken or non-vital teeth, pets are often much happier than those with these teeth left in their mouths. Extraction therapy means the function of that tooth will be lost, but once the extraction site is healed, there should be no residual pain.
Making the Right Decision
The most important issue is that our pets do not need to live with painful teeth and/or broken teeth, and therefore these decisions should not be neglected. The decision whether to perform endodontic therapy or extraction therapy should be made in consultation with a veterinarian and is often based upon several factors including the overall health and age of the patient, the ability of the patient to safely undergo anesthesia, the extent of damage to the tooth, which tooth is involved and the cost of the procedures. Leaving a fractured tooth with pulp exposure in a pet’s mouth is not considered a humane option, however.
—————————————-
About Stephen Riback, DVM
Dr. Riback received his veterinary degree from the New York State College of Veterinary Medicine at Cornell in 1985. He was a general practitioner from 1985 until 1999 and owned the Oakdale Veterinary Hospital from 1989 until 1999. Dr. Riback has worked at the AMC since 1999, first in the Community Medicine dept. and then from 2003 in the Dentistry dept. where he studied dentistry under the mentorship of Dr. Dan Carmichael, who is the only board certified veterinary dentist in New York City.
The department of dentistry is the only full service veterinary dental practice in New York City and operates Monday through Friday at the AMC. Dr. Carmichael works on Mondays and Dr. Riback is in Tuesday through Friday. Dental procedures and oral surgeries are performed Monday through Friday.