Oncology
About Oncology at AMC
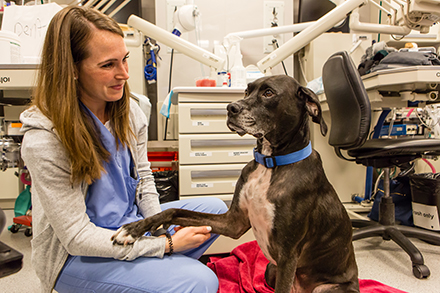
AMC’s Cancer Institute is a revolutionary medical center, created to provide integrative and comprehensive care for pets diagnosed with cancer. This innovative design enables our staff to deliver on the Institute’s core mission – to care for more animals, focus on early detection, maximize the amount of time owners can spend with their beloved pets, and work toward a cure through advanced research. Because we believe that our best friends deserve the best chance.
The primary function of the Oncology Service is to treat cancer in pets with a goal of curing their disease. We also provide palliative treatment and end of life care. The most common tumors treated at AMC are: lymphoma, mast cell tumors, feline injection site sarcomas, osteosarcoma, soft tissue sarcoma, and mammary gland tumors, but any pet with any type of cancer can be cared for by the Oncology Service.
The Oncologists at the Schwarzman Animal Medical Center are board certified by the American College of Veterinary Internal Medicine in recognition of their training and knowledge in caring for pets with cancer. They regularly participate in teaching rounds at AMC and Memorial Sloan Kettering Cancer Center in order to hone their cutting-edge skills and further their objective of providing the best quality of life for pets suffering from cancer.
Our Approach
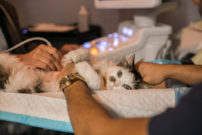
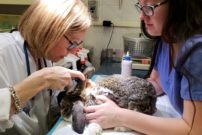
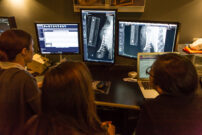
Cancer diagnosis and treatment is greatly enhanced by a team approach through collaboration with our Specialists in Internal Medicine, Pathology, Surgery, Diagnostic Imaging, and Radiation Oncology.
Our Specialists strive to minimize side effects and optimize tumor reduction to achieve a remission and provide your pet with the best possible quality of life.
Treatment
In some cases, surgical removal of tumors, either alone or in combination with other treatments, can control cancer and provide the best quality of life for your pet. Other pets may benefit from the following routinely administered treatments:
- Chemotherapy
- Immunotherapy
- Radiation therapy
- Investigational therapies (recently an investigational program involving the vaccination of dogs with melanoma has achieved success)