Blog
What AMC’s New Surgical Institute Means for Your Pet
With great fanfare, the Schwarzman Animal Medical Center held a “leash cutting” ceremony to mark the grand opening of the Denise and Michael Kellen Institute for Surgical Care. The press release describes...
Read More-
Cats EmergencyMay 15, 2024
Behind the Scenes at the ER: A Foster Kitten’s Night at AMC
Regular readers of my blog will know that my family and I have raised numerous foster kittens over the years. We have had queens and kittens, kittens without moms and infant kittens...
Read More -
Pets and FamilyMay 08, 2024
Keep Kids Engaged with Animal-Based Activities This Summer
Summer is just around the corner, and many parents will be looking for activities to occupy their children while school is out. For children fascinated by animals, there are a whole host...
Read More -
SurgeryMay 01, 2024
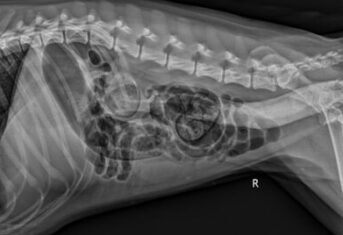
Torsion and Volvulus in Dogs, Cats and Rabbits
Most people don’t realize it, but internal organs are not fixed in place and do have the ability to move around inside the body. When the movement of an internal organ involves...
Read More
-
CatsApril 24, 2024
Why does my cat eat plants? Does it help with hairballs?
Hairball Awareness Day is celebrated on the last Friday in April. This year it falls on April 26th. Like many cat owners, I find hairballs one of the more annoying facts of...
Read More -
Vet LifeApril 17, 2024
AMC Celebrates Client Services Appreciation Week 2024
During Client Services Appreciation Week, April 21-27, 2024, the Schwarzman Animal Medical Center celebrates the many accomplishments and diverse roles of our Client Service Team. This 75-person team allows veterinarians like me...
Read More -
Pet Safety Responsible Pet OwnershipApril 10, 2024
How Should I Dispose of My Pet’s Old Medications?
If you’ve ever had a sick pet, you probably have a cabinet full of unused medications. In fact, I know you do, because my clients often ask if they can give the...
Read More