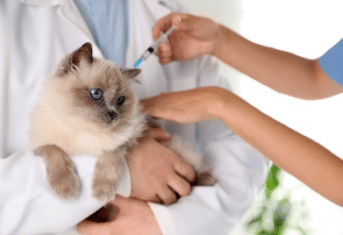
Arthritis in Your Pet
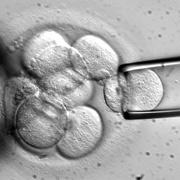
Arthritis in Your Pet
What is arthritis?
Arthritis is “doctor speak” for inflammation of one or more joints. It can be caused by infections such as Lyme disease or other tick borne organisms. Uncommonly, aberrant responses of the immune system to medications, or unknown factors also causes arthritis in multiple joints at the same time. By far the most common cause of arthritis in dogs is due to injury to the cranial cruciate ligament (the cause of football knee in humans) or as a result of the developmental abnormality known as hip dysplasia. These forms of arthritis are often referred to as osteoarthritis. Most dog owners are aware of the possibility of osteoarthritis in their pets; however, veterinarians are just now beginning to diagnose osteroarthritis in older cats.
How is arthritis diagnosed?
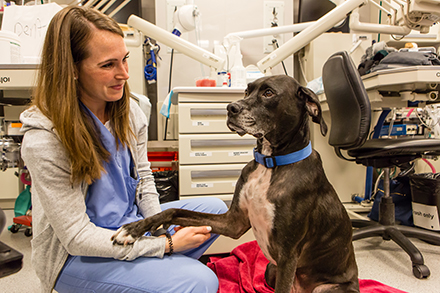
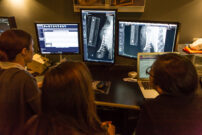
You may be the first to suspect a diagnosis of arthritis in your pet. You may notice she is not moving around as much as usual or he is not racing to the door to greet a returning family member. Your dog may cut short her favorite walk or your cat may develop a limp. A routine annual physical examination by your veterinarian will give additional clues to the diagnosis. He may detect a swollen joint, elicit pain during examination and feel crunching when the joints are manipulated. An x-ray will confirm the diagnosis.
How can arthritis be treated?
The main management strategy for osteoarthritis is exercise, diet and administration of analgesic medications and your veterinarians can determine if some or all of these interventions are right for your dog.
Exercise has a dual purpose in the management of arthritis. First, it facilitates weight loss. Overweight pets suffer more from arthritis than pets of an ideal body weight. Second, exercise will strengthen muscles which have become weak due to the inactivity resulting from the pain of arthritis. Your veterinarian may recommend rehabilitation therapy to strengthen muscles around the affected joint to improve function. Never undertake an exercise program in your pet without first consulting with your veterinarian. Your veterinarian can check the AMC website for posters which contain examples of exercises for both cats and dogs.
Diet also plays a dual role in the management of arthritis. Certain pet foods have been formulated to support joint health. These foods contain glucosamine, chondroitin sulfate to promote improved joint function. They also contain optimized ratios of fatty acids which help to decrease inflammation in arthritis joints. If your veterinarian determines your pet is overweight, she may recommend a diet formulated to promote weight loss, which will improve your pet’s ability to get around.
As recently as 10 years ago, there were very few medications on the market to control the pain of arthritis in dogs and cats. Today, there are multiple non-steroidal anti-inflammatory drug (NSAIDs) available by prescription from your veterinarian. These medications are similar to drugs like ibuprofen and piroxicam for the treatment of arthritis in humans. These have been developed specifically for pets and overcome the toxicity problems with administering human arthritis medications to dogs and cats. These products are available as tablets, chewable pills, liquids and injections to meet the needs of every pet. Pet owners should never administer human arthritis medications to their pet as they can be toxic and result in serious life-threatening illness.
Finally, in some cases where the osteoarthritis is severe, surgery may be of benefit. Damaged ligaments in the joint may result in joint instability and surgical repair of the ligament may improve joint function, slow the progression or arthritis and eliminate pain. Removal of damaged bone may decrease pain and improve joint function, especially in small pets. Replacement of the hip or knee joint is an option in the severely affected pet.
The newest treatment for arthritis in dogs is stem cell therapy. Your dog’s own stem cells are harvested from surgically collected fat. The tissue is specially processed to allow the stem cells to be injected back into your dog. Our next blog will feature information from Dr. Pamela Schwartz, AMC veterinary surgeon, who will discuss her experience with stem cell therapy for arthritis.
_____________________________________
For nearly a century, The Animal Medical Center has been a national leader in animal health care, known for its expertise, innovation and success in providing routine, specialty and emergency medical care for companion animals. Thanks in part to the enduring generosity of donors, The AMC is also known for its outstanding teaching, research and compassionate community funds. Please help us to continue these efforts. Send your contribution to: The Animal Medical Center 510 East 62nd Street, New York, NY 10065. For more information, visit www.amcny.org.
To make an appointment at The AMC, please call 212.838.7053.